Minimally invasive therapies
Alternatives to surgery
Treatments on the spine and joints
The experienced specialists and orthopaedic surgeons at ORTHO EINS are specialists in conservative and minimally invasive treatment approaches. This is why our spine specialists rely on regenerative procedures whenever possible to avoid surgical interventions. ORTHO EINS spine specialists recommend the use of traditional treatment methods such as acupuncture, osteopathy and chirotherapy (manual therapy), but also rely on modern therapy methods such as targeted injections as part of periradicular therapy (PRT).
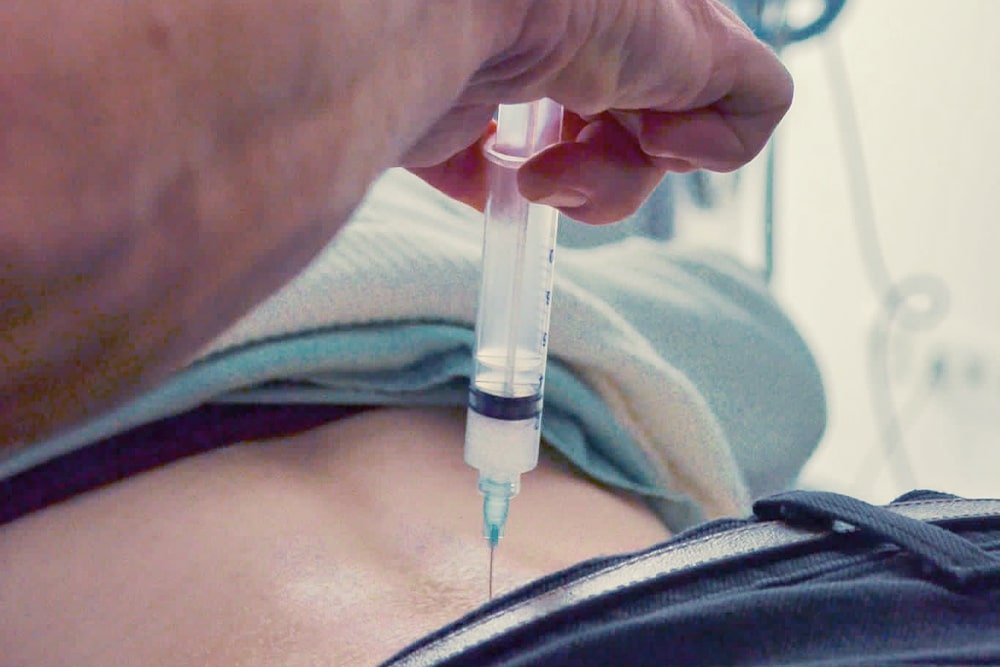
Overview of therapies
Facet injections
Facet injections
The indication for such an injection is facet syndrome. This is a type of pain caused by changes in the small vertebral joints and leads to chronically recurring mechanical back pain.
With facet injections, a special needle is guided to the vertebral joints (facets) to be treated and then advanced through the joint capsule into the vertebral joint. A mixture of local anesthetic, isotonic saline solution and a cortisone preparation is injected into and around the joint. The injection takes place under vision with the aid of an image intensifier. The facet injections are carried out two to three times at intervals of 5-7 days.
Transforaminal epidural injections
Transforaminal injections
In a transforaminal injection, the medication is administered together with a contrast medium under visual control in the immediate vicinity of the spinal nerve causing the pain and its root.
Here too, a second injection is given at the same site every 5-7 days. Indications for a transforaminal injection are pain patterns with a radicular spread, i.e. a pain distribution that can be precisely assigned to a specific nerve, its course and the structures it supplies.
Ramus injections
Ramus injections
Performing a ramus injection (ramus: Latin for “branch”, branch of a small nerve root, i.e. the smallest nerve) is both a diagnostic and therapeutic precision procedure. In this procedure, nerve branches that sensitively innervate the facet joints are injected with a small amount of local anesthetic. If there is a significant reduction in pain or freedom from pain for a short time afterwards, these vertebral joints or the nerves supplying them are responsible for the pain symptoms. If the procedure does not change the symptoms, the source of the pain must be different.
The main indication for a diagnostic medial branch block (small branch of a nerve) is to find out whether the complaints can be attributed to these facet joints, which are innervated by these nerves. If the medial branch block is positive (pain-free for a short time), we use radiofrequency therapy, for example. For ramus injections, we inject a mixture of saline and steroids in addition to the local anesthetic, which has an anti-inflammatory effect.
Denervation and nerve ablation
Denervation and nerve ablation
At our ORTHO EINS practice, we offer nerve ablation, a modern, minimally invasive treatment option for patients with chronic pain in the back, sacroiliac joint, knee, hip, or shoulder. This therapy is particularly suitable when conservative measures such as medication, physiotherapy, or injections no longer provide sufficient relief.
ISG injections
ISG injections
For diagnostic injections into the sacroiliac joint, a local anesthetic is injected into the sacroiliac joint suspected to be the cause of your back pain. The inflammation underlying your pain can have many causes – such as a metabolic disorder, age-related wear and tear and lack of exercise, but also overloading, for example through sport or sports injuries. The team of specialists at Dr. Topar ORTHO EINS specializes in identifying the cause of your back pain and taking effective medical countermeasures. This pain is common in rheumatism and after fusion operations.
After the anesthetic has been injected into your sacroiliac joint, you will be asked to pay attention to any changes in your pain symptoms. If there is no relief of the symptoms, the injected joint can be ruled out as the cause of the pain. If you are completely pain-free for a short time, the source of the pain has been identified and further treatment can be started. In such a therapeutic SI joint injection, which in some cases is performed after the diagnostic SI joint injection, cortisone is added to the anesthetics to achieve an immediate anti-inflammatory and decongestant effect. A further injection is usually required after one week.
HOW EXACTLY DOES AN INJECTION INTO THE SACROILIAC JOINT WORK?
You position yourself face down on a table during the diagnostic or therapeutic SI joint injection. A cushion under your stomach provides comfort and brings your back into the desired position. A doctor from our back specialists in Berlin will use touch and fluoroscopy, which is X-rays of your pelvis, to find the right spot for the SI joint injection. This is also possible with ultrasound control without radiation.
First, your skin and the underlying tissue up to the sacroiliac joint are anesthetized with a local anesthetic. Your doctor will now inject a medication into the sacroiliac joint through the anesthetized area. The needle is then removed and a small plaster is applied. After this outpatient medical treatment, you can leave our practice without any problems.
ISG INJECTIONS: RISKS & SIDE EFFECTS
A diagnostic or therapeutic SI joint injection for back pain, also known as infiltration, is a safe method that involves comparatively few risks. However, these cannot be completely ruled out.
Even if the risks and pain associated with an SI joint injection cannot be completely kept away from you, our team of experienced specialists will ensure that these are minimized as far as possible. We do our best to make diagnostic and therapeutic SI joint infiltrations as comfortable as possible.
Caudal injections
Caudal injections
For a caudal injection, you lie on a couch in a prone position. The lower opening of the spinal canal, which is located in the sacrum (so-called sacral hiatus), is identified with the help of a C-arm (image intensifier). After surgical disinfection and sterile covering, we insert a needle into this opening of the spinal canal under local anesthesia, through which a contrast agent is administered. We observe this process with the image converter in real time. If the agent is distributed in the spinal canal as expected, the saline-steroid mixture can be injected. Once the injection is complete, you will remain in a prone position for a further 2-3 minutes to allow the injected medication to spread further in the spinal canal. We carry out the injection again at intervals of one week.
Use for back pain
Caudal injections are used by back specialists for a variety of painful lumbar syndromes (lower back pain) with different causes. Possible reasons for an injection are pain caused by disc protrusions/herniations, vertebral joint inflammation or scarring, surgical interventions and narrowing of the spinal canal (spinal canal stenosis) in the lower two disc segments (L4/5 and L5/51).
Discography
Discography
Discography is used to search for the cause of pain in the intervertebral discs, as these can also be the cause of chronic pain. MRI or CT scans often do not reveal any major abnormalities. In this case, it may be discogenic pain.
Here we use the discography to verify the suspected diagnosis. Under sterile conditions, antibiotic shielding, local anesthesia and under visual control, needles are inserted into three intervertebral discs until the tip of the needle reaches the nucleus pulposus. Once the exact position of the needle tip has been determined, contrast medium is applied to the intervertebral disc nucleus, thereby provoking an increase in pressure. During this procedure, we ask the patient several times whether the known pain occurs (memory pain).
If the pain can be reproduced by the increase in pressure in the intervertebral disc – in terms of intensity, quality and spread – this provides a decisive indication of the intervertebral disc to be treated. Once the discography has been completed, a CT scan can be performed. Here we can see how the injected contrast medium has spread and – depending on the result – discuss further treatment options.
The procedure is low-risk and is performed under local anesthesia by a back specialist.
Diagnostic test infiltrations
Diagnostic test infiltration
In diagnostic test infiltration, only a local anesthetic is injected into the desired area. Within the next few hours, we observe one of the following changes in the patient: complete temporary pain relief, pain reduction or no change compared to the patient’s previous condition.
The source of the pain is identified as soon as you are pain-free for the duration of the anesthetic. We can then initiate the next therapeutic step. The situation is different when the pain subsides: In this case, the anesthetized area causes some of the pain, but other sources of pain are still present. These are then searched for by means of test infiltration, which is used in step-by-step diagnostics.
A clear diagnosis cannot initially be made either by describing the symptoms or clinical examination or by imaging procedures (X-ray, MRI or CT).
Injections under ultrasound
Injections under ultrasound
In our practice, we offer the advanced and completely low-radiation procedure of ultrasound injections. An imaging procedure is essential for the exact positioning of the needle tip and the precise administration of an injection. In addition to the image intensifier, ultrasound technology is ideal for this process. Injections in the joints and spine are carried out very precisely and without radiation exposure.
Catheter technology
Catheter technology
In this procedure, we place a cannula under local anesthesia in the desired neuroforamen (bony constriction in the spinal canal). A slightly curved catheter is inserted through this cannula and carefully advanced under visual control. Finally, it comes to rest between the nerve root and the intervertebral disc. This is followed by the administration of contrast medium to verify the position of the catheter tip. The product is finally distributed. Adhesions and chemically toxic processes that form around the nerve root through contact with the fluid from the core of the intervertebral disc (nucleus) are stretched, loosened, neutralized and flushed away with saline solution and medication. This precise therapy enables the optimum effect to be achieved.
After treatment, there is temporary numbness and loss of strength in the leg on the side of the lumbar spine that was injected. The patient then lies on a cooling element in the relaxation room for about 10-20 minutes. As the anesthetic wears off, normal sensitivity and the usual strength of the leg are restored. Instructions are then given on specific back exercises, a cooling bandage for the lumbar spine and anti-inflammatory medication.
The gentle procedure offers several advantages, as general anesthesia and incisions are not necessary. The catheter technique is used by back specialists for unilateral, radicular pain triggered by various causes (e.g. herniated disc).
Radiofrequency therapy (RFT)
Radiofrequency therapy (RFT)
Radiofrequency therapy is a therapeutic procedure in which probes are positioned on nerves that supply a specific painful facet joint or sacroiliac joint . The pain is caused by degenerative changes or inflammation in the small vertebral joints to the right and left of the spinous process, which are known as facet joints due to their arrangement. If the distance between the vertebrae changes, for example due to wear and tear, the facet joints can no longer function properly and begin to cause pain.
This can result in incorrect loading, which can lead to facet syndrome and thus to chronic back pain. A sports injury can also result in facet syndrome, which our specialists treat using RFT.
The painful nerve is heated by a precisely placed probe and thus destroyed. The outpatient method is low-risk, gentle on the tissue and very effective. General anesthesia is not required.
The prerequisite for radiofrequency therapy is a positive blockage of the nerve branches. Before deciding on the form of therapy, the back specialists in Berlin identify the nerve branches to be treated by means of a diagnostic test infiltration of the corresponding nerves with a locally injected anesthetic.
HOW EXACTLY DOES RADIOFREQUENCY THERAPY FOR BACK PAIN WORK?
At the start of radiofrequency therapy in our orthopaedic practice in Zehlendorf, you will lie on your stomach and may be given a relaxing medication. Your skin and the underlying tissue are first anesthetized with a syringe. One of our orthopaedic specialists inserts a narrow cannula and guides it to the source of the pain under visual control using X-rays. These nerves transmit the pain impulses from the facet joints in the spine to the brain.
An electrode is now passed through the cannula to these nerves and their position is checked with a weak energy impulse. The radio frequency current passed through the needle then heats the nerve, thereby destroying its function of transmitting pain impulses. If the pain is not only transmitted by one nerve, it is necessary to repeat the treatment on the other nerves as well.
Immediately after the outpatient treatment, you will receive a small plaster on the treated area. After a short time you can go home. The treated area may feel a little sore and your pain will not be gone immediately after the treatment. Ideally, your back pain will disappear over the course of the next few weeks.
Methylene blue injection
Methylene blue injection
Originally discovered and used as a dye, over time methylene blue found more and more applications in the field of medicine. It is now also used in the treatment of chronic low back pain caused by degenerative changes in the intervertebral discs that cause pain (discogenic pain). In the case of discogenic pain, nerves have grown into the degenerated intervertebral disc.
Under sterile conditions, a spine specialistinserts a needle into the disc to be treated while constantly monitoring the position of the cannula/catheter. Once the needle has found its exact position in the intervertebral disc, a small amount of methylene blue is injected. As a neurotoxic substance, methylene blue destroys nerves in the damaged intervertebral disc. This can provide pain relief.
Intradiscal electrothermal therapy
Intradiscal electrothermal therapy
The minimally invasive procedure is usually performed for chronic pain in the intervertebral disc. Nerve fibers can grow into the damaged disc ring and cause discomfort. IDET is used to heat and destroy the altered nerves. To do this, we insert a flexible heating probe via a precisely positioned cannula into the outer ring of the disc to be treated and then heat the probe. The temperature increases continuously. As soon as the target temperature of 85°C is reached, it is maintained for a few minutes.
Intradiscal electrothermal therapy usually takes place under local anesthesia. Thanks to local anesthesia, we can communicate with you. You will be given an antibiotic to minimize the risk of infection. IDET is performed sterile and under visual control, is very low-risk and gentle.
Joint injections
Joint injection
For the treatment of acute pain in all joints (e.g. knee or shoulder joint), we apply the active ingredient in the highest possible concentration directly to the source of the pain. The type of substance injected depends on the diagnosis previously made. Cortisone preparations in combination with a local anesthetic or autologous blood preparations are most commonly used for joint complaints, which are usually degenerative, inflammatory or rheumatic in nature.
Treatment is carried out with or without imaging, depending on the joint to be treated and the injection agent used. Experience has shown that two to three injections should be administered at weekly intervals in order to combat the cause of the symptoms and achieve the longest possible treatment success.
Joint irrigation/lavage
Joint lavage
In degenerative, arthritic joints, cartilage particles are worn away, among other things. This can lead to chronically recurring irritation caused by friction (sometimes with effusion formation). Inflammatory cells accumulate in the synovial fluid of the diseased joint. As a result of the cell proliferation, the synovial membrane becomes inflamed and thickens. Joint adhesions form. In this case, the minimally invasive procedure of joint irrigation can lead to significant pain relief or even freedom from symptoms with little effort. Joint irrigation is also useful for post-traumatic and post-operative complaints. We usually perform joint irrigation on the knee, hip, shoulder and ankle joints.
Under sterile conditions and local anesthesia, a cannula is inserted into the joint cavity. To ensure the correct position of the needle, we use an image intensifier to inject contrast medium over the positioned cannula and view the distribution on the screen. If it runs inside the joint capsule, the cannula is in the correct position and lavage can begin. Sterile saline solution is injected into the joint to increase the pressure in the joint capsule. Adhesions are loosened and the capsule is widened. If the pressure in the joint is so great that the capsule can no longer expand, we allow the irrigation fluid to flow out again via the unchanged needle. Cartilage debris and mucous membrane particles are removed. This process is repeated until the draining liquid has been cleaned.
A mixture of cortisone and local anesthetic as well as hyaluronic acid or an autologous blood preparation is then injected into the joint to inhibit inflammation and build up cartilage, and the cannula is removed. You will then receive two to four more injections of hyaluronic acid into the rinsed joint. These take place at intervals of one week.
Supplementary and interdisciplinary services
Complementary and interdisciplinary services
Long-lasting or permanent pain leads to a reduction in quality of life and a change in mood. As medical or physiotherapeutic treatment methods are often not sufficient, we offer our patients accompanying psychological support (coaching). Learning to deal with your own problems or finding ways to make it easier to deal with the pain are just some of the goals of such coaching. We offer our patients an initial consultation in our practice rooms to get to know each other.
Issuing certificates
Issuing certificates
A certificate is required, for example, for exemption from school sports or for medically necessary training breaks at the gym. In thorough examinations we convince ourselves of the necessity of a medical certificate. If your physical health does not permit sporting activities, we will be happy to issue you with one at any time. In certain cases, the joints and bones should be spared so that the illnesses do not become more serious.


